Tumor Metastatic Model Development Service
Metastasis is the process by which cancer cells migrate through lymph or blood vessels, leading to the formation of new tumors in distant organs. It is the primary cause of death in the majority of bladder cancer cases. At Alfa Cytology, we specialize in providing our clients with tumor metastatic models specifically designed for bladder cancer research.
Introduction to Metastatic Bladder Cancer
In muscle-invasive bladder cancer, approximately 25 percent will either have metastases at the time of diagnosis or develop metastases later on. The most common sites of metastasis in bladder cancer include the lymph nodes, lungs, liver, and bones. Local infiltration and peripheral lymph node metastasis are more frequently observed in bladder cancer metastasis, while distant metastasis occurs less frequently.
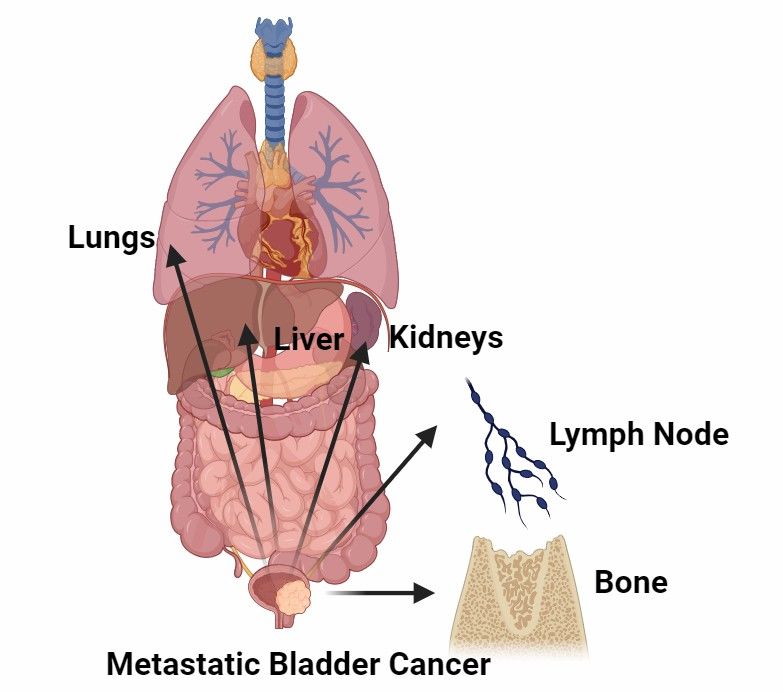
Although metastasis is the cause of most bladder cancer-related deaths, the mechanisms of metastatic disease are not yet fully understood, in part due to the lack of preclinical in vivo models. The development of advanced preclinical models of metastasis will help us understand bladder cancer progression and develop new therapies for metastatic bladder cancer.
Our Services
Alfa Cytology, a leading provider of preclinical contract research organization (CRO) services, specializes in tumor metastatic model development for bladder cancer. Our services include but are not limited to:
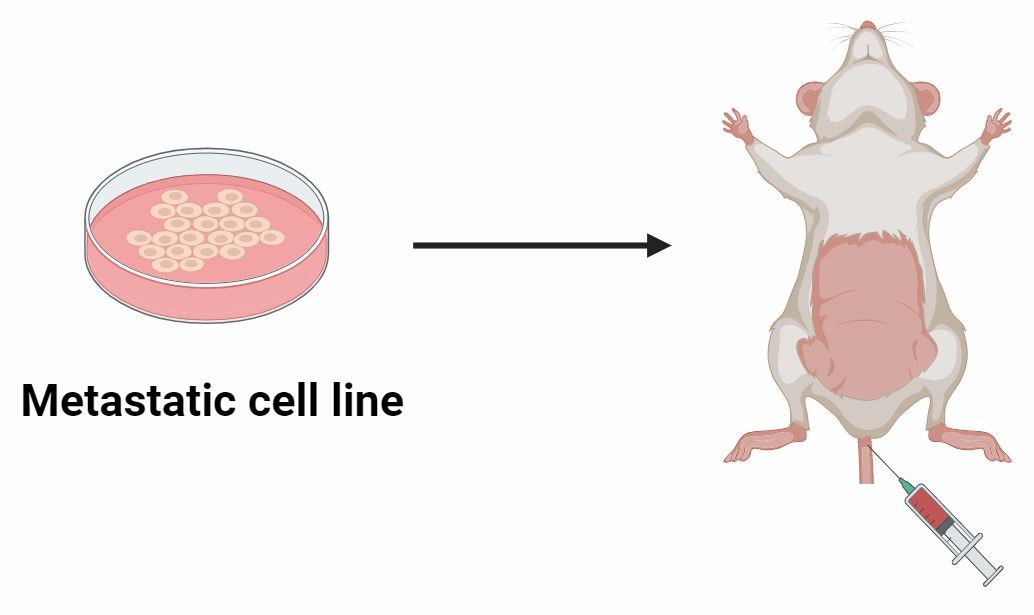
| Development of Orthotopic Mouse Models |
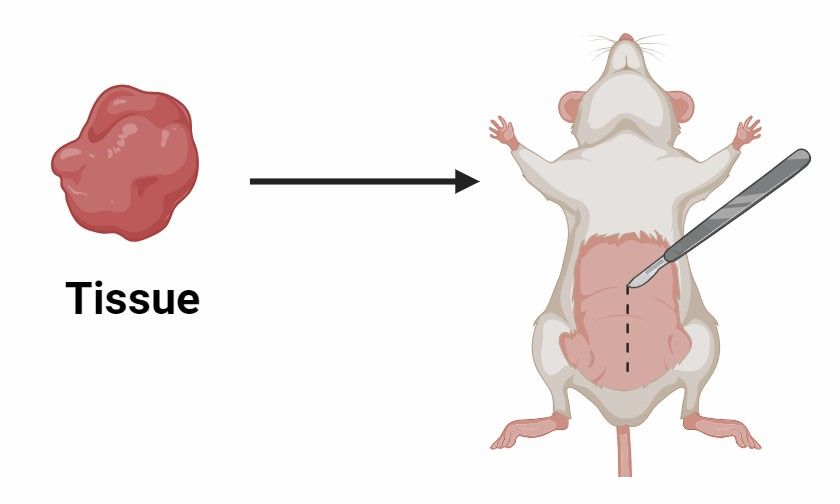
Development of Patient-Derived Xenografts (PDX) |
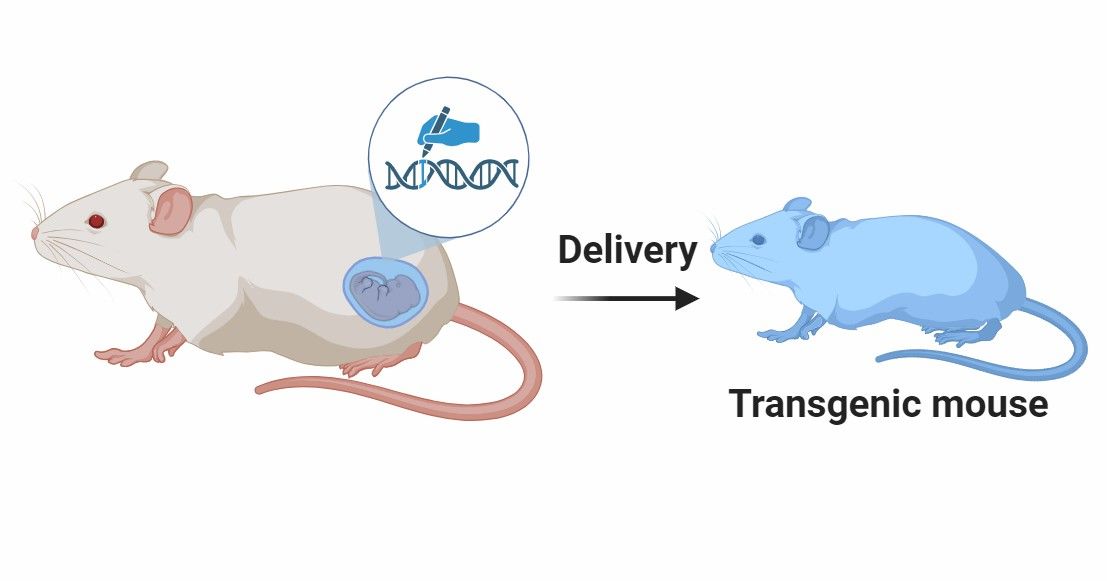
Development of Genetically Engineered Mouse Models |
|
 |
 |
 |
| By implanting bladder cancer cells directly into the bladder wall of mice, we recreate the complex interactions between tumor cells and the bladder microenvironment. |
Our PDX service involves the transplantation of patient-derived tumor tissue or cells into immunocompromised mice. This enables the preservation of the genetic and phenotypic characteristics of the original patient tumor. |
We specialize in the development of GEMMs for bladder cancer research, where specific mutations or alterations associated with bladder cancer are introduced into mice. |
Our Services Will Help You Achieve the Goals as Follows:
Orthotopic Mouse Models
- Relevance to the human microenvironment, closely mimicking the characteristics of human bladder tumors.
- Ability to study local invasion, intravesical spread, and distant metastasis observed in human.
- Investigation of metastatic processes and identification of potential biomarkers.
PDX
- Preservation of genetic and phenotypic characteristics of the original tumor.
- Investigation of tumor heterogeneity and individualized therapy responses.
- Identification of predictive biomarkers and evaluation of therapeutic efficacy.
Genetically Engineered Mouse Models
- Study of specific genetic alterations associated with bladder cancer.
- Investigation of molecular mechanisms underlying bladder cancer metastasis.
- Analysis of the interplay between genetic alterations, tumor microenvironment, and metastatic progression.
- Insight into the spontaneous development of bladder tumors and metastases.
Case Study - Orthotopic Model of Bladder Cancer with Spontaneous Renal Metastasis
Model Introduction
The RT112-luc bladder-renal metastasis orthotopic model provides a specialized and highly relevant preclinical platform for studying the metastatic progression of human bladder urothelial carcinoma to the kidney, a clinically significant site of metastasis. This model leads to efficient and reproducible formation of primary bladder tumors and subsequent spontaneous kidney metastasis.
Model Information
- Model: RT112-luc Bladder-Renal Metastasis Orthotopic Model
- Animals: BALB/c Nude Mice
- Age: 7-8 Weeks
Model Construction
The RT112-luc bladder-renal metastasis model was established by orthotopic bladder wall injection of RT112-luc human bladder cancer cells into BALB/c nude mice. Each mouse received an injection of 2×10⁶ cells in a volume of 20 µL suspended in 30% matrigel. Primary tumor growth and kidney metastasis were monitored longitudinally via bioluminescence imaging from week 1 to endpoint.
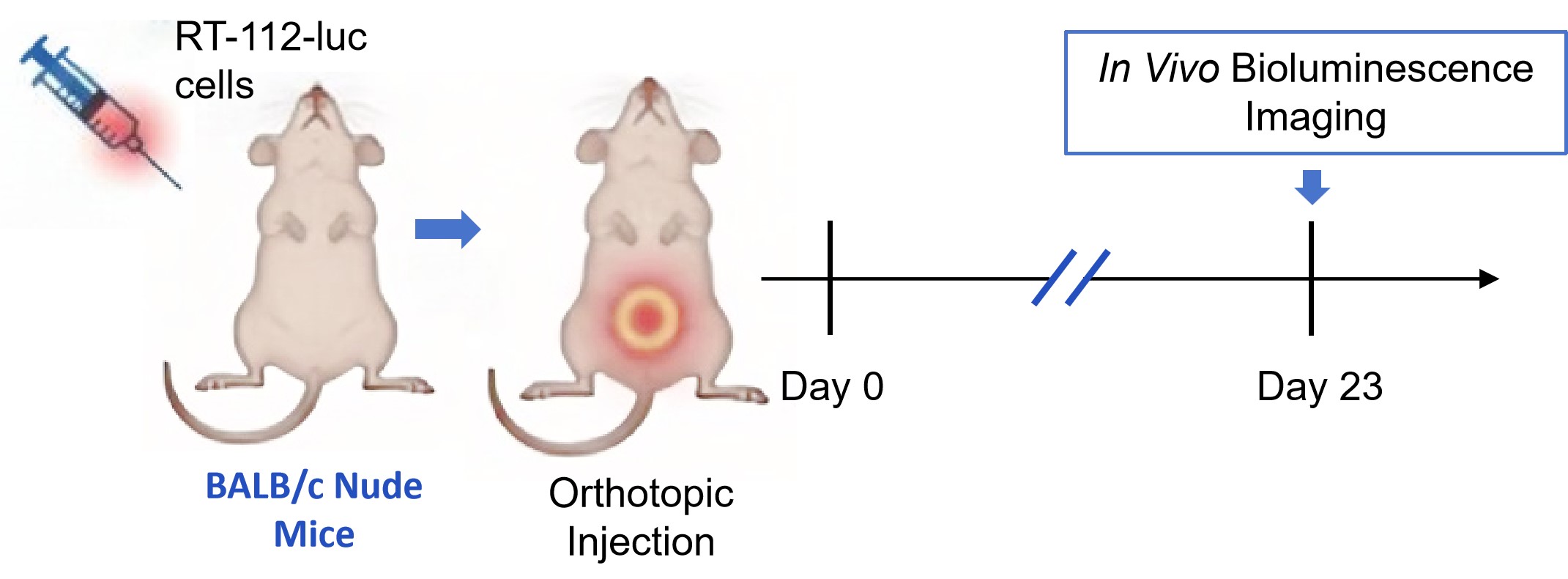 Fig. 1 Workflow of RT112-luc bladder-renal metastasis orthotopic model establishment. (Source: Alfa Cytology)
Fig. 1 Workflow of RT112-luc bladder-renal metastasis orthotopic model establishment. (Source: Alfa Cytology)
Model Data
- Metastatic Establishment & Kinetics: Following orthotopic injection of 2×106 RT112-luc cells, robust and reproducible primary bladder tumor growth and spontaneous kidney metastasis are observed. Kidney metastatic foci are typically detectable via in vivo imaging by 4-6 weeks post-injection, with an incidence rate exceeding 70%.
- Multi-Organ Metastasis Profile: Ex vivo organ imaging confirms a distinct metastatic pattern, with the strongest signals in the kidneys, followed by ureter, lung, liver, peritoneum, and uterus.
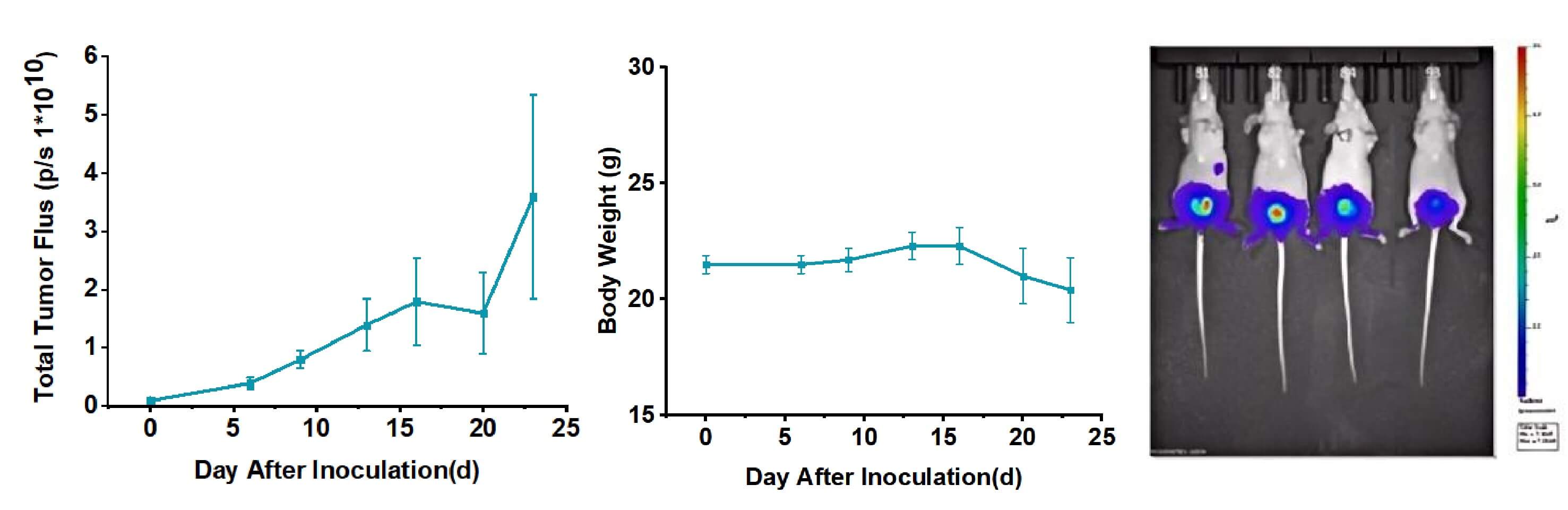 Fig. 2 Metastatic progression and ex vivo validation of the orthotopic RT112-luc bladder cancer model. Data are presented as mean ± standard error (SEM). (Source: Alfa Cytology)
Fig. 2 Metastatic progression and ex vivo validation of the orthotopic RT112-luc bladder cancer model. Data are presented as mean ± standard error (SEM). (Source: Alfa Cytology)
Contact Us
At Alfa Cytology, we are committed to providing comprehensive preclinical CRO services in the field of bladder cancer research. Our tumor metastatic model development service offers advanced orthotopic mouse models, PDX, and genetically engineered mouse models tailored to the study of bladder cancer metastasis. Our team of experts is dedicated to accelerating your research projects, enabling early diagnosis, and developing effective therapeutics strategies for bladder cancer. If you have any needs, please contact us.
Reference
- Tatum, J.L., Kalen, J.D., and et al. A spontaneously metastatic model of bladder cancer: imaging characterization. J Transl Med. 2019, 17, 425.
For research use only. Not intended for any clinical use.
Related Services





 Fig. 1 Workflow of RT112-luc bladder-renal metastasis orthotopic model establishment. (Source: Alfa Cytology)
Fig. 1 Workflow of RT112-luc bladder-renal metastasis orthotopic model establishment. (Source: Alfa Cytology)  Fig. 2 Metastatic progression and ex vivo validation of the orthotopic RT112-luc bladder cancer model. Data are presented as mean ± standard error (SEM). (Source: Alfa Cytology)
Fig. 2 Metastatic progression and ex vivo validation of the orthotopic RT112-luc bladder cancer model. Data are presented as mean ± standard error (SEM). (Source: Alfa Cytology) 